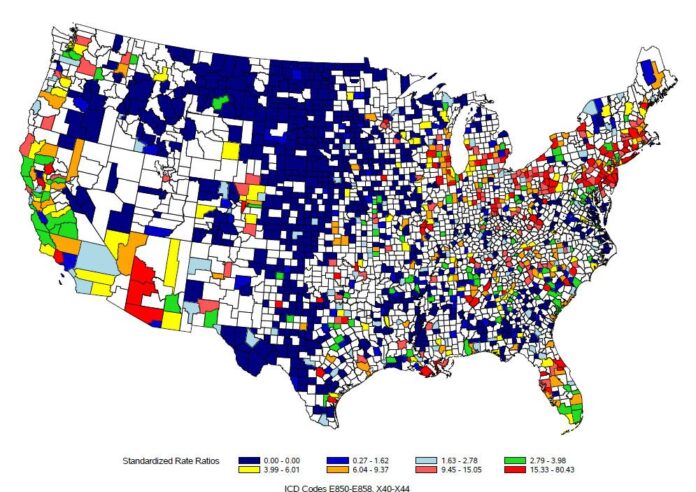
A newly released analysis from Sadaka Law is forcing a sharper national conversation around one of the most persistent and often misunderstood public health challenges in the United States: accidental poisoning deaths. While frequently associated with isolated incidents, the data presents a far more systemic issue, revealing geographic concentrations where fatalities linked to alcohol, narcotics, and medication misuse are occurring at disproportionately high rates. The findings do more than rank counties—they expose patterns that demand a deeper examination of prevention, access to care, and the evolving risks embedded in everyday life.
Across the country, accidental poisoning has steadily climbed into the category of leading causes of injury-related death, a shift driven largely by the intersection of prescription drug availability, illicit substance use, and the widespread normalization of alcohol consumption. What distinguishes this latest data is its precision. By identifying the counties experiencing the highest fatality rates, the study highlights not just where the crisis is most acute, but also where intervention strategies are either failing to keep pace or have yet to be effectively deployed.
This is not a distant issue for New Jersey. In fact, the state sits at a critical crossroads within the broader national trend. With its dense population, extensive transportation networks, and proximity to major metropolitan areas, New Jersey faces a unique set of vulnerabilities that mirror—and in some cases amplify—the conditions seen in the hardest-hit counties. The implications extend well beyond emergency response. They touch healthcare infrastructure, community outreach, mental health services, and the daily decisions individuals make around substance use and medication management.
The data underscores three primary drivers behind accidental poisoning deaths: alcohol-related toxicity, narcotic overdoses, and complications arising from prescription or over-the-counter medications. Each category represents a distinct but interconnected risk profile. Alcohol, often perceived as the most socially acceptable substance, continues to contribute to a significant share of fatalities, particularly when combined with other depressants or used in high quantities over short periods. Narcotics, including both prescription opioids and illicit drugs, remain the most visible component of the crisis, but the study makes clear that they are only part of a much broader equation. Medication-related incidents—ranging from dosage errors to dangerous drug interactions—are emerging as an increasingly significant factor, particularly among older populations and individuals managing multiple health conditions.
For New Jersey residents, these findings align closely with ongoing discussions within the state’s health and wellness ecosystem. Coverage across Explore New Jersey’s health and wellness category has consistently emphasized the importance of preventative care, education, and early intervention. What this study adds is a sense of urgency and specificity. It is no longer sufficient to address substance use as a generalized issue; targeted, data-driven strategies are required to reduce risk at the community level.
One of the most critical takeaways from the report is the role of accessibility—both in terms of substances and healthcare resources. Counties with elevated poisoning death rates often share common characteristics: higher availability of prescription medications, increased presence of illicit drug markets, and gaps in access to addiction treatment or mental health services. In some cases, socioeconomic factors compound these challenges, limiting individuals’ ability to seek help before a crisis occurs. In others, the issue is one of awareness, where individuals underestimate the risks associated with substances they use regularly.
New Jersey’s response framework has evolved in recent years, with expanded access to naloxone, increased public awareness campaigns, and a growing network of treatment providers. However, the study suggests that continued adaptation is essential. The nature of accidental poisoning is constantly changing, influenced by shifts in drug composition, prescribing practices, and consumer behavior. Synthetic opioids, for example, have introduced a level of unpredictability that complicates both prevention and treatment efforts. At the same time, the rise of poly-substance use—where multiple drugs or alcohol are consumed together—has created scenarios where traditional risk assessments may no longer apply.
Beyond the clinical and policy dimensions, there is a cultural component that cannot be ignored. The normalization of certain behaviors, particularly around alcohol and prescription medication use, plays a significant role in shaping outcomes. In many cases, individuals do not perceive themselves to be at risk until it is too late. This disconnect between perception and reality is one of the most challenging barriers to overcome, requiring sustained efforts in education and community engagement.
The Sadaka Law data also highlights the importance of localized solutions. While national trends provide context, effective intervention must be tailored to the specific conditions of each region. For New Jersey, this means leveraging its existing healthcare infrastructure while addressing gaps that may exist in underserved areas. It also means fostering collaboration between public agencies, private organizations, and community groups to create a more cohesive response system.
Technology and data analytics are poised to play an increasingly important role in this effort. Real-time monitoring of overdose incidents, predictive modeling, and improved data sharing between institutions can enhance the ability to identify emerging hotspots and respond proactively. At the same time, these tools must be complemented by human-centered approaches that prioritize trust, accessibility, and cultural competence.
The broader significance of the study lies in its ability to reframe accidental poisoning as a multifaceted issue that extends beyond any single category of substance or behavior. It is a convergence of medical, social, and economic factors, each contributing to an environment where risk can escalate rapidly. Addressing it requires a level of coordination and commitment that matches its complexity.
For readers and communities across New Jersey, the message is clear: awareness alone is not enough. The data demands action, whether through policy changes, community initiatives, or individual choices. The state has already demonstrated a capacity for innovation in health and wellness, and the challenge now is to build on that foundation with strategies that are as dynamic and adaptive as the problem itself.
As this issue continues to evolve, it will remain a central focus within the broader conversation about public health in New Jersey. The findings from Sadaka Law provide a critical benchmark, offering both a warning and an opportunity—to confront the realities of accidental poisoning with clarity, precision, and a renewed commitment to protecting lives across the state.